Many women notice a pattern: symptoms intensify during stressful periods. PMS becomes more painful, cycles feel irregular, mood shifts are sharper, and perimenopausal symptoms flare.
Read more: Is It My Hormones... Or Is It Stress?
This pattern is not coincidental. It reflects a biological interaction between the immune system, the endocrine system and the stress response.
Inflammation as a Hormonal Disruptor

Inflammation is a tightly regulated immune process designed to protect the body. However, when inflammatory signalling becomes chronic, it begins to interfere with endocrine communication¹.
Pro-inflammatory cytokines, including interleukin-6 (IL-6) and tumour necrosis factor alpha (TNF-α), can influence ovarian steroidogenesis and alter oestrogen and progesterone dynamics². Oestrogen itself has complex immunomodulatory effects, capable of both enhancing and dampening immune activity depending on context².
This bidirectional relationship means that hormonal fluctuations can influence inflammatory tone, while inflammation can disrupt hormonal balance. Elevated inflammatory markers have been associated with more severe PMS, endometriosis progression and mood disturbances³.
Read more: Endometriosis and Chronic Pelvic Pain.
In endometriosis, for example, inflammatory mediators contribute to lesion growth, pain sensitisation and altered local oestrogen metabolism³. In perimenopause, declining and fluctuating oestrogen may shift immune balance, potentially increasing susceptibility to inflammatory symptoms.
The HPA Axis and Cortisol
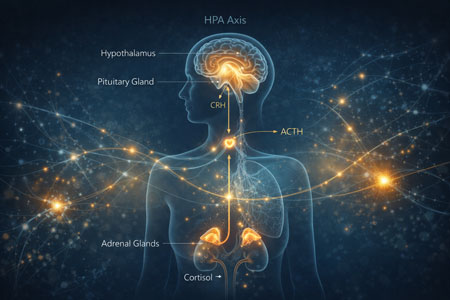
The stress response is coordinated through the hypothalamic–pituitary–adrenal (HPA) axis. When psychological or physiological stress occurs, cortisol is released to mobilise energy and maintain short-term survival⁴.
Acute cortisol release is protective. Chronic activation, however, produces different outcomes.
Persistently elevated cortisol can:
Disrupt hypothalamic–pituitary–ovarian (HPO) axis signalling.
Suppress ovulation or alter cycle regularity.
Promote visceral fat accumulation (which itself secretes inflammatory cytokines).
Impair sleep architecture.
Chronic psychological stress has been shown to promote sustained inflammatory activity, even when overt infection is absent⁵. This creates a physiological loop: stress elevates cortisol, prolonged cortisol dysregulates immune signalling, immune activation increases inflammation, and inflammation disrupts hormone regulation.
Additionally, inflammation sensitises peripheral and central pain pathways, which may explain why stress exacerbates pelvic pain and menstrual cramping³.
The Endocannabinoid System as a Regulatory Bridge
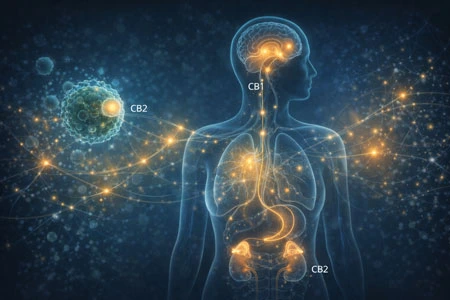
The endocannabinoid system (ECS) plays a modulatory role in stress adaptation and immune regulation. Cannabinoid receptors (CB1 and CB2) are present in the central nervous system and immune cells, where they influence inflammatory signalling and neurotransmission⁶.
The endocannabinoid system (ECS) plays a modulatory role in stress adaptation and immune regulation. Cannabinoid receptors (CB1 and CB2) are present in the central nervous system and immune cells, where they influence inflammatory signalling and neurotransmission⁶.
Preclinical and clinical research suggest the ECS helps buffer excessive stress responses and limit overactivation of inflammatory pathways⁶. Dysregulation of endocannabinoid tone has been proposed in conditions characterised by chronic pain and inflammatory imbalance.
While research continues to evolve, understanding the ECS highlights an important principle: the body contains intrinsic regulatory systems designed to restore homeostasis.
A Systems-Based Perspective
Hormonal symptoms rarely arise from a single pathway. They reflect a networked interaction between:
Immune signalling
Neuroendocrine stress pathways
Ovarian hormone dynamics
Metabolic and sleep regulation
When stress load decreases, inflammatory signalling often follows. When the inflammatory burden reduces, endocrine communication can stabilise.
Rather than viewing worsening symptoms as random, it is more accurate to understand them as biologically responsive.
And responsiveness means modulation is possible, through stress reduction, sleep optimisation, anti-inflammatory lifestyle patterns, and evidence-informed therapeutic guidance.
The goal is not to eliminate inflammation, but to restore balance within an interconnected system.
References
Furman D, et al. Chronic inflammation in the aetiology of disease. Nature Medicine. 2019.
Straub RH. The complex role of estrogens in inflammation. Endocrine Reviews. 2007.
Bulun SE. Endometriosis. New England Journal of Medicine. 2009.
Smith SM, Vale WW. The role of the HPA axis in neuroendocrine responses to stress. Dialogues in Clinical Neuroscience. 2006.
Slavich GM, Irwin MR. From stress to inflammation and major depressive disorder. Psychological Bulletin. 2014.
Di Marzo V. The endocannabinoid system in inflammatory and immune responses. Nature Reviews Immunology. 2011.
Disclaimer: This blog supports responsible cannabis use. The information contained in this article is for educational and informational purposes only and is not intended as health or medical advice. Always consult a physician or other qualified health provider regarding any questions you may have about a medical condition or health objectives.