Hormones Are Responsive – Not Random
Women’s hormones are frequently described as unpredictable. In reality, they are responsive signalling molecules influenced by sleep, metabolic stability, inflammation and stress physiology.
Across a typical menstrual cycle, oestrogen rises during the follicular phase, supporting energy, cognition and tissue growth. After ovulation, progesterone increases, contributing to mood stability, thermoregulation and sleep quality. When this rhythm is disrupted, symptoms such as intensified premenstrual syndrome (PMS), irregular cycles, worsened pain sensitivity, or perimenopausal instability may occur.
Chronic stress is one of the most significant disruptors of this rhythm.
The Stress–Hormone Axis
Activation of the hypothalamic–pituitary–adrenal (HPA) axis increases cortisol production. Sustained cortisol elevation can interfere with gonadotropin-releasing hormone (GnRH) signalling, ovulatory function and progesterone balance¹. Stress exposure is also associated with sleep disturbance and increased inflammatory signalling². Both of which may amplify hormonal symptoms.
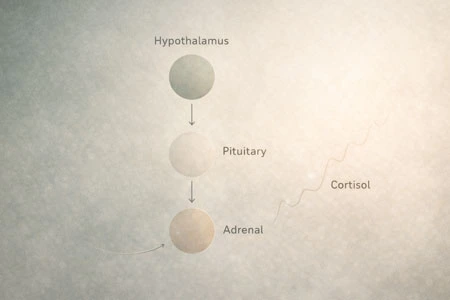
What is often labelled “hormone imbalance” may, in many cases, reflect chronic nervous system activation.
The Endocannabinoid System and Reproductive Function
The endocannabinoid system (ECS) plays a central role in maintaining homeostasis. It consists of cannabinoid receptors (CB1 and CB2), endogenous ligands such as anandamide, and metabolic enzymes that regulate their synthesis and degradation³.
Read more: The Endocannabinoid System.
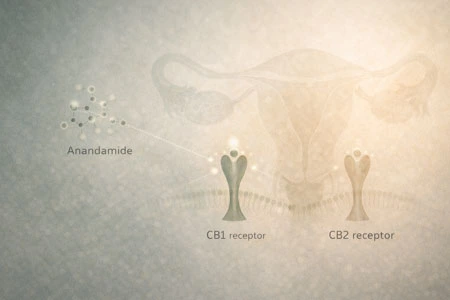
The ECS influences stress recovery, immune regulation and nociceptive processing. Importantly, it is also active within reproductive tissues. Endocannabinoid signalling has been identified in the ovaries, uterus and placenta, with evidence suggesting that fluctuations in endocannabinoid tone occur across the menstrual cycle⁴.
Read more: The Menstrual Cycle and the Endocannabinoid System (ECS).
Oestrogen appears to modulate ECS activity, indicating a bidirectional relationship between reproductive hormones and cannabinoid signalling pathways⁵. This interaction may partly explain why stress-related dysregulation can manifest as both mood and menstrual disturbances.
Where Cannabinoids May Fit
Plant-derived cannabinoids interact with this endogenous system. Cannabidiol (CBD), a non-intoxicating cannabinoid, has been studied for its potential role in modulating anxiety and stress reactivity pathways⁶. Preclinical and clinical data also suggest cannabinoids influence pain processing and inflammatory cascades⁷.

However, cannabis is not a hormone replacement therapy. It does not directly increase oestrogen or progesterone levels. Its proposed relevance in women’s wellness lies in regulatory support. Particularly around stress modulation, sleep quality and pain perception.
Read more: Cannabis for Women: A Naturally Ally for Hormonal Harmony.
Careful titration, awareness of individual response variability and medical guidance remain essential. Additionally, cannabis use is not recommended during pregnancy due to potential developmental risks⁸.
A Regulatory, Not Replacement, Perspective
Emerging research supports a broader framework: reproductive hormones, stress physiology and the endocannabinoid system function as an interconnected network rather than isolated systems.
Read more: Cannabis and Homeostasis.
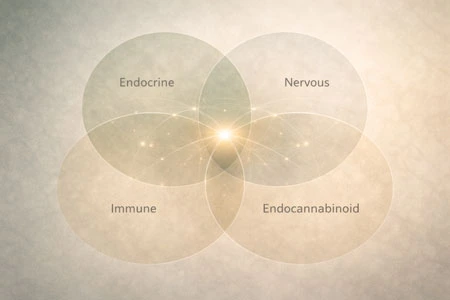
Lifestyle factors, including sleep consistency, micronutrient sufficiency, blood sugar stability and stress management, significantly influence both endocrine and endocannabinoid tone. Where legally accessible and clinically appropriate, cannabinoid-based interventions may represent one component of an integrative strategy.
Read more: Balanced and Buzzing.
Understanding this interconnected physiology allows for a more nuanced, evidence-informed discussion of cannabis in women’s hormonal health, grounded in regulation rather than oversimplification.
References
Chrousos, G.P. (2009). Stress and disorders of the stress system. Nature Reviews Endocrinology, 5(7), 374–381.
Touma, C., & Palme, R. (2005). Measuring faecal glucocorticoid metabolites in mammals and birds. Annals of the New York Academy of Sciences, 1046, 54–74.
Lu, H.C., & Mackie, K. (2016). An introduction to the endogenous cannabinoid system. Biological Psychiatry, 79(7), 516–525.
El-Talatini, M.R. et al. (2009). The endocannabinoid system in reproductive tissues. Human Reproduction Update, 15(5), 501–513.
Gorzalka, B.B., & Dang, S.S. (2012). Minireview: Endocannabinoids and gonadal hormones. Endocrinology, 153(3), 1016–1024.
Blessing, E.M. et al. (2015). Cannabidiol as a potential treatment for anxiety disorders. Neurotherapeutics, 12(4), 825–836.
Vučković, S. et al. (2018). Cannabinoids and pain: New insights. Frontiers in Pharmacology, 9, 1259.
Gunn, J.K.L. et al. (2016). Prenatal exposure to cannabis and maternal and child health outcomes. BMJ Open, 6(4), e009986.
Disclaimer: This blog supports responsible cannabis use. The information contained in this article is for educational and informational purposes only and is not intended as health or medical advice. Always consult a physician or other qualified health provider regarding any questions you may have about a medical condition or health objectives.