There’s something strangely consistent about waking up at 3 AM. Not 1 AM. Not 5 AM. But right in the middle of the night. Alert, restless, and often unable to fall back asleep. While it may feel random, this pattern is rarely accidental. It’s usually your body communicating something deeper. Linked to your hormones, metabolism, and natural sleep architecture. Let’s unpack what’s really happening.
Your Sleep Is Not One Continuous State
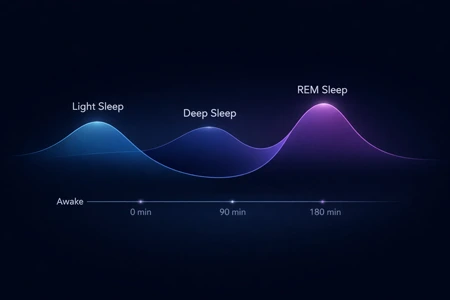
Sleep happens in cycles, each lasting about 90 minutes. These cycles move between light sleep, deep sleep, and REM (dream) sleep.¹ Around 2–4 AM, your body transitions through lighter sleep phases. This makes you more sensitive to internal changes. Like shifts in hormones or blood sugar. So if something is slightly “off,” you’ll feel it then.
Cortisol: The Early Morning Signal

Cortisol is often called the “stress hormone,” but it’s also essential for waking you up and regulating your circadian rhythm. Under normal conditions:
- Cortisol is lowest at night
- Begins rising in the early morning (around 3–4 AM)
- Peaks shortly after waking²
But when your system is under stress, mental, physical, or metabolic, this rhythm can shift. Instead of a gentle rise, you may get a spike. That spike can wake you up. Common triggers include:
- Chronic stress or anxiety
- Overstimulation before bed
- Poor sleep habits
- Nervous system dysregulation
Your body is essentially saying: “It’s time to be alert.” Even when it isn’t.
Blood Sugar Drops While You Sleep

Another overlooked cause of waking at 3 AM is blood sugar instability. During the night, your body continues to use glucose for essential functions. If your blood sugar drops too low, your body responds by releasing cortisol and adrenaline to bring it back up.³ This process can:
- Wake you suddenly
- Increase heart rate
- Create a sense of alertness or anxiety
This is more likely if:
- You skipped dinner
- Ate high-sugar or refined carbs before bed
- Have underlying insulin resistance
- Are under prolonged stress
In this case, waking up is not a sleep problem; it’s a metabolic response.
The Liver Time Theory (Traditional Perspective)

In Traditional Chinese Medicine, 1–3 AM is associated with the liver, an organ responsible for detoxification and emotional processing. While this isn’t a Western scientific framework, it reflects an interesting overlap: the liver plays a key role in blood sugar regulation and metabolic balance during the night. So whether viewed traditionally or biologically, this window is a time of internal activity.
Your Nervous System Might Still Be “On”

If your nervous system hasn’t fully shifted into a parasympathetic (rest-and-repair) state, sleep can remain shallow and easily disrupted.⁴
This often shows up as:
- Falling asleep easily but waking suddenly
- A racing mind in the early hours
- Feeling “tired but wired”
Modern lifestyles, constant stimulation, late-night screen use, and emotional load make this increasingly common.
Supporting Deeper, More Stable Sleep

Rather than forcing sleep, the goal is to support the systems behind it.
Consider:
- Eating a balanced dinner with protein, healthy fats, and complex carbs
- Avoiding excessive sugar or alcohol before bed
- Creating a consistent wind-down routine
- Reducing blue light exposure at night
- Supporting nervous system regulation (breathwork, gentle stretching, calming rituals)
For some individuals, plant-based support such as CBD or calming adaptogens may help regulate the stress response and promote a more stable sleep cycle, though responses vary and should be approached thoughtfully.
A Different Way to Understand Night Waking
Waking at 3 AM isn’t your body failing. It’s your body responding. To stress. To blood sugar. To rhythm disruptions. When you understand the signals, you can work with your system, not against it.
If your sleep feels unpredictable, fragmented, or difficult to understand, you don’t have to figure it out alone. Our free and confidential consultation is designed to help you explore what your body may be signalling, and guide you toward safe, personalised support options.References
- Carskadon MA, Dement WC. Normal human sleep: an overview. Principles and Practice of Sleep Medicine. 2017.
- Clow A, et al. The cortisol awakening response: more than a measure of HPA axis function. Neuroscience & Biobehavioral Reviews. 2010.
- Cryer PE. Mechanisms of hypoglycaemia-associated autonomic failure. New England Journal of Medicine. 2013.
- Thayer JF, Lane RD. Claude Bernard and the heart–brain connection. Neuroscience & Biobehavioral Reviews. 2009.
Disclaimer: This blog supports responsible cannabis use. The information contained in this article is for educational and informational purposes only and is not intended as health or medical advice. Always consult a physician or other qualified health provider regarding any questions you may have about a medical condition or health objectives.